Posted by Bassem Gerges in Blog, Gynaecology, Obstetrics on April 14th, 2020
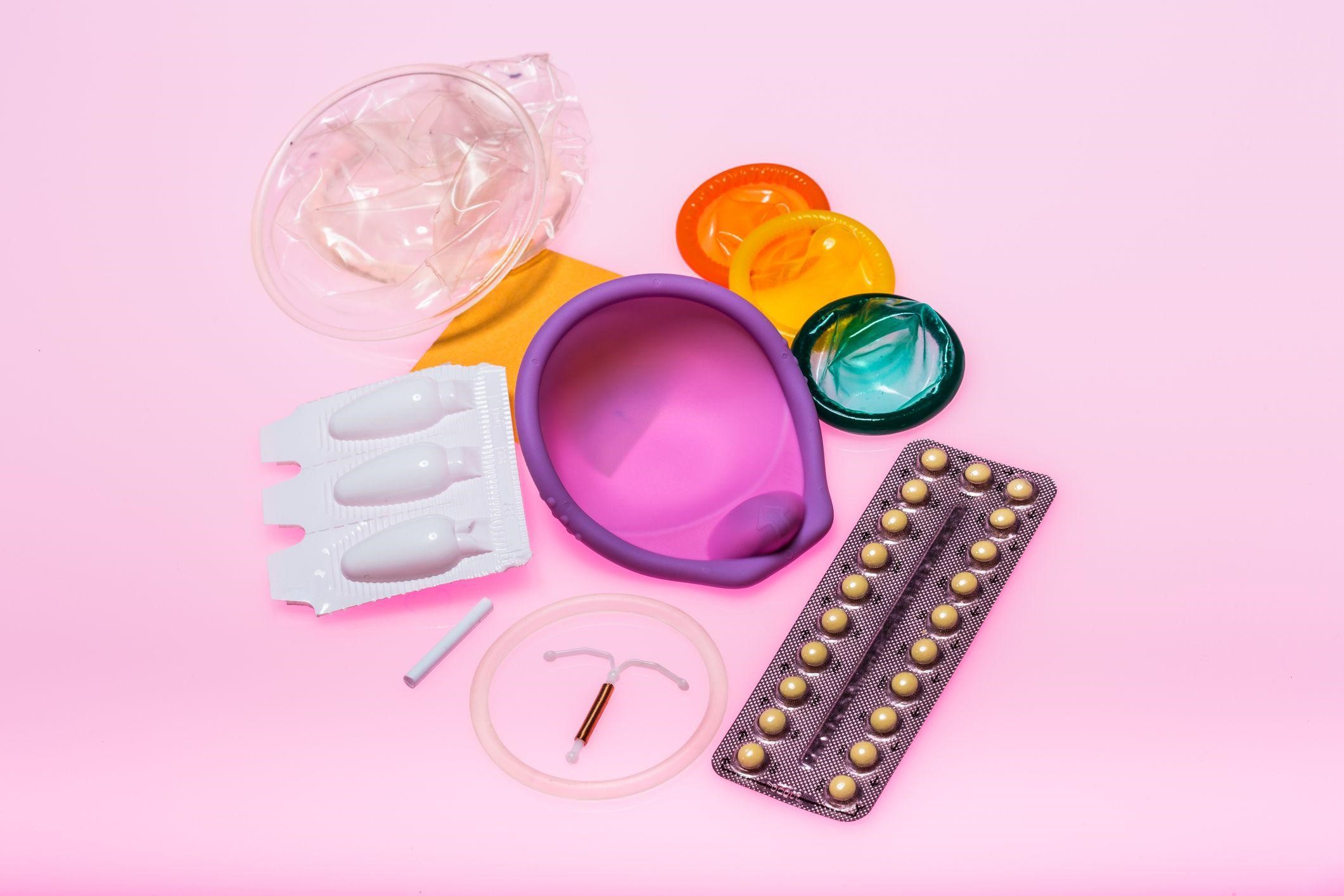
Contraception is a highly personal choice that every woman should be informed about. No method will suit everyone, however it’s important to dispel any misinformation about contraception, so that you can make a safe and effective choice.
At Norwest Obstetrics & Gynaecology, Drs Gerges and Wilson pride themselves on providing you with the most up-to-date scientific information about contraception and your reproductive health, so that you can make an informed decision.

Although Intra-uterine Devices (IUDs) are a safe and very effective form of protection from pregnancy, only 7% of Australian women use an IUD. This compares to 21% of Swiss women and 17% of French women.
An IUD is a small copper or plastic object that is inserted into a woman’s uterus to prevent sperm from fertilising an egg.
The IUD is a cheap, safe and effective method of contraception that has been around since the 1970’s. However, Australian research has found that there are a number of myths that have prevailed in the community about the safety of the IUD, which have historically made this an unpopular contraception choice.
Several high profile cases in the U.S. 30 years ago, of pelvic infection and subsequent infertility, were related to the strings of one type of IUD. However modern devices don’t increase the risk of infection. Yet this myth about the safety of IUDs continues to live on.
One 2010 study of 996 women by Family Planning Queensland found that 95% of all IUD insertions were successful, with 90% of these insertions reported as being easy by the doctor.
Although it’s important to remember that an IUD won’t protect you against getting a sexually transmitted infection.
The most popular form of contraception in Australia is the combined oral contraceptive pill. Worldwide this is also the case with around 100 million women taking the pill.
The “pill” switches off a woman’s natural production of the hormones, progesterone and oestrogen. These are replaced by synthetic versions of both hormones. These synthetic hormones inhibit the release of eggs from the ovaries and alter the lining of the womb, so that implantation of the fertilised egg is less likely.
Although the pill is effective in preventing pregnancy, there are also other prescribed benefits and reasons why women take it. The pill can be used to regulate your periods and reduce severe menstrual pain. It can also be effective in reducing the symptoms of conditions like polycystic ovarian syndrome and endometriosis.
One pervasive myth about the pill, is that it will reduce a woman’s ability to conceive a child, after she’s taken the pill for a long period of time. Research shows that most women want to return to their pre-pill fertility levels when they cease taking the pill.
Yet some women find it difficult to fall pregnant after stopping the pill. This leads women to conclude that the contraception affects their long-term fertility. However, the factors that affect a woman’s fertility are far more complex than this.
It’s challenging to assess the effects of the pill on a woman’s fertility, when many other factors are at play. Fertility is affected by a woman’s age, concurrent illnesses, weight, exercise levels, cigarette smoking and stress levels. A review of studies found that between 79% and 96% of women were able to get pregnant after 12 months of actively trying and ceasing taking the pill.
There is limited evidence to suggest that using the pill for contraception has a long-term impact on fertility. Although it is very effective for women wanting to prevent pregnancy in the short term.
Research indicates that on average, women will take the pill for three to five years. Although this average duration will vary from country to country.
Recent studies from Australia and the U.S. have found that many women worry that taking the pill will lead them to store up hormones in their bodies, leading to problems. This erroneous idea has led to the common misconception that women should take a break from the pill every once in a while.
Some women attribute the side effects of breast tenderness, headaches, nausea and bloating to the pill itself. Although these symptoms occur as a result of the hormone free interval. This interval allows the withdrawal bleed to occur, mimicking the natural menstrual cycle.
The reproductive health specialists at Norwest Obstetrics & Gynaecology will make a detailed medical assessment of your health to establish whether or not you would be suitable for the contraceptive pill, and if so, what kind. The pill is not suitable for everyone and so an individualised assessment is essential. Drs Bassem Gerges and Matthew Wilson will be able to help you find the right pill that suits your needs.

Many medications have a small risk of serious side effects associated with them. This is also the case with the contraceptive pill. The risk of adverse side effects is highest when you resume taking the pill after a break and also in the first few months of taking it.
Whilst research has shown that there is a slightly elevated risk of cervical cancer associated with taking the pill, there has also been evidence that it reduces your risk of endometrial and ovarian cancer.
One of the most serious side effects associated with the pill is an increased risk of thrombotic complications such as stroke, myocardial infarction, and venous thromboembolism (VTE). These are also known as blood clots in the heart, brain, limbs and groin. These risks are more serious for women who smoke or who are in mid-life and have a risk of heart disease.
Although these risks are serious, the risk of blood clots is low. The risk is marginally higher compared to women not taking the pill. To put the research into perspective, when you take the pill, your risk of blood clots is lower than the risk of blood clots during pregnancy, delivery and post-partum.
There are other forms of effective contraception aside from the pill, known as Long Acting Reversible Contraception (LARC). Although Australian media stories in recent years have focused on isolated cases of women who have experienced adverse side effects from using LARC such as contraceptive implants (Implanon) and IUDs (Mirena).
These media stories failed to show how the majority of women who use a LARC, find these methods reliable, effective and easy. Adverse side effects and complications arising from the use of Implanon affect less than 1 in 1,000 women.
One U.S. study involving 10,000 women found that when they were provided with evidence based information about the LARC and when financial barriers to purchase were removed, that over 70% of the women chose LARC.
A large study in the U.S. (the CHOICE study) involving more than 7,000 women showed, when provided with evidence-based information, more than two-thirds of women chose a LARC over other methods.
One reason to support the use of LARC is that these methods don’t require daily adherence to be effective. This makes these contraception methods ideal for young women who have high fertility and are susceptible to unwanted pregnancy.
It’s vital that you have regular checks with an Obstetrician/Gynaecologist. Your contraceptive needs will change as you grow older. This is particularly the case as you reach milestone points in your reproductive life such as becoming sexually active, getting into a long-term relationship with someone, trying to conceive, after having a child and when you’ve completed your family. No matter what stage you are at, the team at Norwest Gynaecology & Obstetrics are always here for you! Call us on 02 8883 5143 or request an appointment on our website.
American Journal of Obstetrics and Gynaecology (2010) The Contraceptive CHOICE Project: reducing barriers to long-acting reversible contraception.
Monash University (2012) Monday’s medical myth: the pill affects long-term fertility. Professor Sonia Davison, The Conversation.
La Trobe University (2018) No, women don’t need to ‘take a break’ from the pill every couple of years, Professor Jayne Lucke, The Conversation.
La Trobe University (2012) IUDs safe, effective but myths live on The Conversation.
The University of Sydney (2017) Reporting a few cases of negative side effects from long-acting contraceptives is alarmist and damaging, Professor Kirsten Black, The Conversation.
Posted by athena in Blog, Gynaecology, Obstetrics on August 30th, 2019

“Eat up – remember you’re eating for two now!”
“Be careful, it’s difficult to lose weight after you give birth.”
“Don’t worry, once you start breastfeeding, the weight will drop off you”
Pregnant women are often bombarded with conflicting advice about what they should eat and the optimal weight they should maintain for their baby’s and their own health. In our first blog post, Norwest Obstetrics & Gynaecology will clarify the current scientific research on this important topic.

Many women simply trust their appetite when it comes to eating during pregnancy. They don’t eat a specially designed diet and will eat what tastes good for them or what feels right at the time. However if you find yourself eating foods high in fat, salt and sugar, it may be time to consider replacing these foods with healthier options like fresh fruits and vegetables. Doing 30 minutes of moderate exercise 3-4 times per week (for example swimming, yoga or walking), can also help to keep weight down.
The Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG) recent guideline provides the following advice regarding weight gain for women during pregnancy

However, your BMI is not the only factor that influences health outcomes for you and your baby. At Norwest Obstetrics & Gynaecology we can help you to gain a complete picture of your baby’s health. Our highly experienced Obstetricians Drs Matthew Wilson and Bassem Gerges provide exceptional medical care. Every woman’s body, health and lifestyle is different. We provide compassionate and supportive medical care that is tailored to your personal journey towards motherhood.
Your body will change rapidly during pregnancy to ensure that your unborn child gets the nutrients and water they need. A lot of these changes begin at conception and happen behind the scenes, then become noticeable as time goes on. You will gain a lot more weight in the final few months of pregnancy, compared to first few months. The additional weight isn’t only the growing baby, it’s your biological support system that is sustaining the baby’s growth. This includes the baby’s circulation, the placenta and amniotic fluid.
For example, if at full term, your baby weighs approximately 3 – 3.5 kg (7-8 lbs). The rest of your pregnancy weight gain will be made up of the following:
If you began your pregnancy at a healthy or normal BMI, then you only need to gain another 0.5-2kg of weight during the first trimester. This is good news if you’re struggling to keep food down because of morning sickness.

Steady weight gain is more important during the second and third trimesters. If you started out at a healthy weight or you are underweight then you should aim to gain at least half a kilo per week until delivery. Simply by adding a sandwich and some fruit or vegetables to your diet each day should help you to achieve this.
Overweight or obese women should aim to gain about 0.2kg per week in the second and third trimesters.
For many years, it has been well-known that smoking and high alcohol consumption during pregnancy can lead to low birthweight, pre-term birth, as well as higher rates of diabetes and heart disease later in life.
Research published in The Lancet found that a woman’s health in the years before she becomes pregnant has an impact her own health during the pregnancy and the baby’s development.

One Australian longitudinal study from 2015 demonstrated that women with a healthy and balanced diet in the three years prior to pregnancy, were less likely to get high blood pressure, gestational diabetes and pre-eclampsia during pregnancy. A balanced diet includes a high intake of fruit, vegetables, legumes, nuts, fish and a low intake of red or processed meats.
Physical activity has a protective role for women and their babies. Higher levels of physical activity before conception leads to a lower risk of pre-eclampsia and gestational diabetes.
If a woman gains more than 0.5 kg of weight each week, then additional tests and examinations may be needed. Extreme weight gain of 1 kg per week can indicate serious health problems, such as pre-eclampsia. The main symptom of this pregnancy-related condition is high blood pressure. This is sometimes accompanied by nausea, headaches and dizziness too. Pre-eclampsia can be life-threatening to both mother and child. Therefore it’s essential that you tell you obstetrician as soon as possible.
Rapid weight gain during pregnancy also increases the risk of women developing gestational diabetes. This can also be a sign that a woman already has gestational diabetes. This is a type of diabetes where blood sugar levels increase in women who didn’t have diabetes prior to becoming pregnant.
Gestational diabetes also increases the risk of pre-eclampsia, and can result in the unborn baby putting on a lot of weight. This can delay the birth and make it more difficult to give birth naturally.

The age of social media ensures that pregnant women are constantly bombarded by (often digitally enhanced) images of celebrities with their perfect post-baby physiques.
This can be damaging to your self-image and mean that you can’t really enjoy the experience of being pregnant and having a large belly. Weight gain is an unavoidable part of being pregnant, but your changing body in all of its wondrous natural capabilities should be celebrated, not become a source of shame.
Every woman’s body, health and lifestyle is different. It’s therefore critical that you get the best medical advice that’s tailored for yourself and your baby. Norwest Obstetrics & Gynaecology are accredited with the Royal Australian and New Zealand College Of Obstetricians and Gynaecologists (RANZCOG). We have received excellent feedback from our patients on our service delivery.
Patient care is our first priority and we give our women the time and attention needed in their scheduled appointments with their chosen doctor. Book an appointment with us today on 02 8883 5143.
RANZCOG Management of Obesity in Pregnancy Guideline
Diabetologia (2015) Pre-pregnancy dietary patterns and risk of gestational diabetes mellitus: results from an Australian population-based prospective cohort study (2015) Danielle A. J et. al.
Institute for Quality and Efficiency in Health Care (IQWiG) (2006) Pregnancy and birth: Weight gain in pregnancy
The Lancet (2018) Preconception Health
The Mayo Clinic (2017) Pregnancy weight gain: what’s healthy?
University of Technology, Sydney (2011) Why it’s a bad idea to eat for two during pregnancy. Dr Caroline Homer. University of Technology, Sydney, The Conversation.
Posted by athena in Blog, Gynaecology, Obstetrics on August 22nd, 2019

Women of all ages are familiar with the sensation of stabbing pain that hails the monthly arrival of their period. This is often described as being stabbing, sharp or cramping pain that ranges from mild to severe. For some women, this pain can be so debilitating that it can disrupt school, work, social and family life. For others, the pain is simply a temporary simple occurrence that can be overcome with over-the-counter pain medication.
So what’s the difference? Drs Bassem Gerges and Matthew Wilson of Norwest Obstetrics & Gynaecology are highly experienced in diagnosing the underlying conditions and causes of period pain. In this article you will discover what may be at the root of your period pain and how Norwest Obstetrics & Gynaecology can help to treat it.
Each month, the uterus prepares itself for pregnancy by growing its thick lining called the endometrium that’s rich in blood supply. This uterine lining awaits implantation by a fertilised embryo.
When fertilisation doesn’t occur, the body produces a period, which is actually the shedding of the endometrium. During this time, the blood vessels in the uterus open and the lining (endometrium) sheds from the uterine wall. The muscles in the uterus contract in order to expel the blood and tissue.
dysmenorrhoea) you experience can be categorised into two types.
Occurs in women with normal pelvic anatomy. 90% of women in Australia who experience period pain are experiencing primary dysmenorrhoea caused by the usual prostaglandin release at the time of their period.
Endometriosis is when cells that are similar to the lining of the womb (endometrium) are deposited outside of the uterus, most commonly on the organs in the pelvis. The hormones in your body that trigger a period also cause bleeding at these sites of implanted endometrial tissue. This causes inflammation and pain which can last not only during your period, but at other times throughout the month. Pain is also a common experience for women with endometriosis during sex and at the time of ovulation. Endometriosis is also associated with infertility. Similarly, adenomyosis, is when endometrial-like cells are in the muscle of the uterus (myometrium), and respond to the hormones from your ovaries as with endometriosis, also causing pain and heavy menstrual bleeding.

The way that women interpret pain in their pelvis varies depending on the person. Some women can have severe endometriosis and have very little or no pain. Whereas other women with minimal or mild endometriosis experience severe pain.
Many women dismiss this pain as being normal and often don’t seek treatment for it. Yet the impact of endometriosis on women’s lives is very real. Many girls and women have to take time off from work or study as a result of the pain. Endometriosis is not a fatal disease, but it does cause ongoing discomfort and pain for women and often disrupts their lives.
The oral contraceptive pill can often help to manage the symptoms of endometriosis. Also progesterone implants (Implanon) or progesterone coated intrauterine devices (Mirena) can be helpful treatment options for reducing the pain of periods. However, these treatments don’t work for everyone.
Dr Bassem Gerges and Dr Mathew Wilson of Norwest Obstetrics & Gynaecology provide appropriate gynaecological treatments and surgery utilising the least invasive laparoscopic (key-hole) methods. This includes high quality gynaecological care for women dealing with endometriosis. They regularly perform laparoscopic (key-hole) surgery and Dr Gerges routinely performs in-office deep endometriosis ultrasound scans.
Many women delay seeing a gynaecologist about their pain and therefore don’t get a proper diagnosis and treatment. This delay can bring with it a lot of anxiety and pain about how they can resolve their issue.
When you visit Norwest Obstetrics & Gynaecology, Dr Gerges and Dr Wilson will do a complete analysis of your medical history and a physical examination. If endometriosis is suspected to be the cause of your pain they will then clearly explain the medical treatment options, the risks and benefits of laparoscopic surgery and tailor an individualised treatment plan to your health needs.
There are several other conditions which lead to pelvic pain. Acyclical or non-cyclical pelvic pain is the kind that occurs on a regular basis (i.e. a few times per week), even when you’re not having your period. There may be many reasons for this. Some of the more common problems are:
It’s worth asking for a referral to Norwest Obstetrics & Gynaecology if you have the following symptoms:
Also, if you just feel as though something is not right,, book an appointment with your GP who can refer you to Norwest Obstetrics & Gynaecology. Dr Gerges and Dr Wilson will be able to discuss a variety of diagnostic investigations with you, in order to find out the cause and provide you with personalised treatment options. Arrange a referral to the clinic or call us on 02 8883 5143.
Mayo Clinic (2019) Menstrual Cramps Symptoms and Causes
The American College of Obstetricians and Gynaecologists (2012) Dysmenorrhoea: Painful Periods Frequently Asked Questions
University of Adelaide (2015) Genders experience pain differently, and women have it more. Dr Susan Evans, Gynaecologist, Pain Medicine Physician, Laparoscopic Surgeon, The Conversation
UNSW (2017) Health Check: are painful periods normal? Dr Rebecca Deans, Paediatric and adolescent gynaecologist at Royal Hospital for Women and Sydney Children’s Hospital, UNSW
Western Sydney University (2018) I have painful periods, could it be endometriosis? Dr Mike Armour Post-doctoral research fellow, Western Sydney University.